1 out of 200 kidney surgery recipients DIE in just 30 days after the procedure, new study warns
05/13/2017 / By Russel Davis
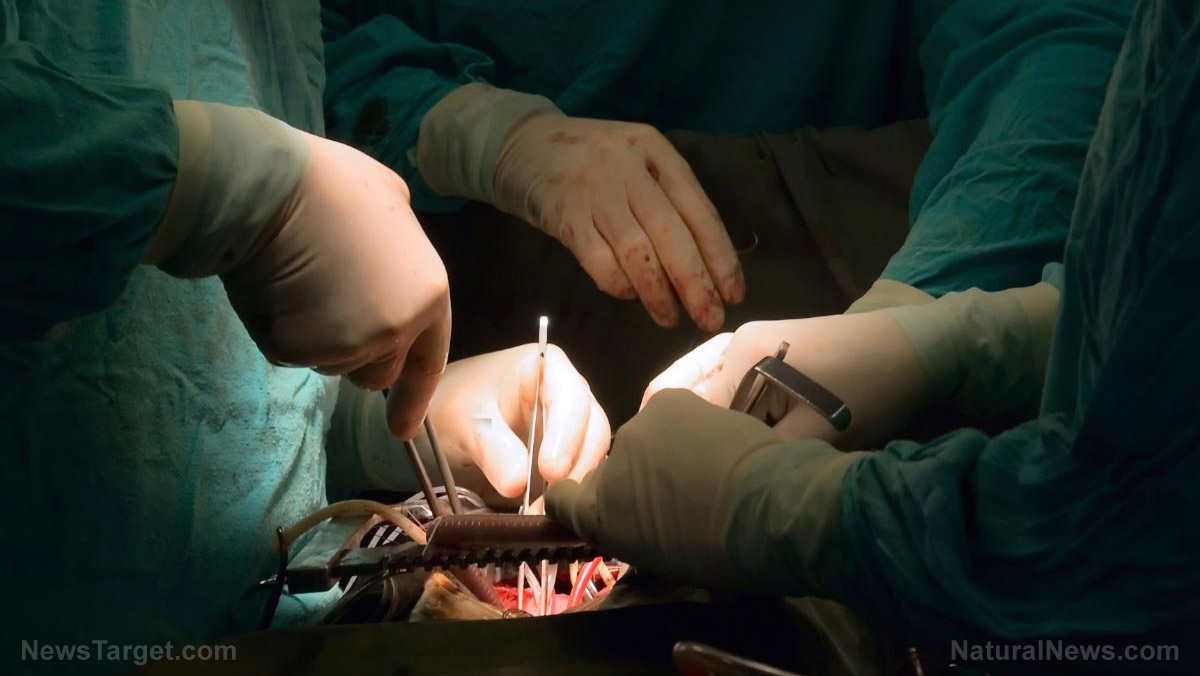
A recent analysis published in the journal BJU International revealed that all forms of kidney surgery were associated with a slight increase in 30-day mortality. As part of the study, a team of British researchers pooled data from the British Association of Urological Surgeons National Nephrectomy Audit with a total cohort population of more than 21,000 kidney surgery patients. The health experts also calculated the risk of 30-day mortality in patients.
According to the meta-analysis, the overall 30-day mortality rate following nephrectomy was 0.5 percent. The researchers also found that radical kidney surgery was associated with a mortality rate of 0.6 percent. The rates of 30-day mortality was 0.1 percent for partial kidney surgery and 0.4 for simple nephrectomy, the health experts added. This number equated to about one in 200 patients dying within a month following kidney surgery.
The review also revealed that old age and pre-existing, comorbid conditions increased the risk of 30-day mortality in kidney surgery patients. Significant blood loss and advanced stages of kidney disease raised the odds of death in patients, the researchers said. The research team also noted that modest blood loss and conversion from minimally-invasive to open surgery served as new risk factors for 30-day mortality following kidney surgery.
“This pan-national study provides fresh insights into the contemporary risk of death following all types of nephrectomy and identifies potential novel risk factors for death. Massive thanks to all the surgeons who contributed their data making this sort of comprehensive study possible,” said lead author Archie Fernando.
Previous studies find link between kidney surgery, 30-day mortality
A large number of studies have previously demonstrated that certain types of kidney surgeries may elevate the risk of 30-day mortality in patients. A study published in the journal European Urology found that partial or radical nephrectomy for localized diseases was associated with a 0.6 percent to 3.6 percent odds of dying within a month. (Related: Take better care of your health when you read the articles on Healing.news).
As part of the study, a team of researchers pooled data from the National Cancer Institute Surveillance, Epidemiology, and End Results database and examined more than 24,000 kidney surgery patients. According to the study, 219 deaths occurred within a month following the procedure. The study found that age was a major contributing factor in 30-day mortality risk, which ranged from 0.5 percent in patients younger than 49 years old to 1.2 percent in patients 80 years and older. The stage of kidney disease was also tied to an increased risk of 30-day mortality, researchers said. In addition, the researchers found that the risk was lower in patients who underwent partial kidney surgery compared with those who had radical nephrectomy.
Another study revealed that surgery volume appeared to impact 30-day mortality risk in kidney surgery patients. To carry out the study, the researchers used data from the Ontario Cancer Registry and identified 433 patients who underwent radical nephrectomy with venous thrombectomy. The study revealed that the overall rate of 30-day mortality at post surgery was 2.8 percent. The research team also found that surgeons who performed single nephrectomy with venous thrombectomy accounted for 14 percent of the cases and had the highest 30-day mortality rates. Surgeons performing more than one surgery had a mortality rat of up to 2.1 percent.
According to the study, procedure year and low surgeon volume served as significant predictors of 30-day mortality in patients. “For radical nephrectomy with venous thrombectomy, surgeon volume predicts short-term mortality, emphasizing the importance of experience in patient outcome. Despite a shift towards high-volume surgeons, 13.8 percent of cases continued to be performed by low-volume providers. If these results are confirmed in other jurisdictions, radical nephrectomy with venous thrombectomy should be regionalized and performed by surgeons who manage these cases regularly,” the researchers wrote in the journal BJU International.
Sources include:
Tagged Under: kidney, kidney health, kidney surgery, mortality risk, nephrectomy