England’s NHS can’t afford Big Pharma: They will only pay for a new Hep C treatment if the patient is cured
09/18/2017 / By Jhoanna Robinson

England’s National Health Service (NHS) is showing signs that it is cash-strapped: It has recently announced that it will no longer automatically shoulder payment for the treatment of its citizens who are Hepatitis C-afflicted; it will only do so once the patient is cured.
Those who are lucky enough to get cured will have their expenses and medication shouldered by a new Hepatitis C drug manufacturer, who has yet to be identified publicly. Also, the new drug, which is given to 10,000 patients a year, has no public information available due to commercial confidentiality.
The move comes amid repeated cuts to NHS’ budget, which has experienced having many of its services thrown out, leaving insured patients to feel as if their health depends on a “postcode lottery.”
According to NHS England Chief Executive Simon Stevens during the NHS Expo conference in Manchester, cutting costs was essential for the NHS to reach its “full potential” by ensuring that it would have the money to afford drugs for future generations. The new deal may set a precedent in holding Big Pharma companies accountable by only compensating for treatments that actually work.
Stevens said the agency plans on saving 300 million pounds a year by 2021 by heightening the uptake of “biosimilar” drugs, which are medications that biotech companies develop after the patents of approved recombinant drugs (for example, erythropoietin, human growth hormone, insulin, interferons, and monoclonal antibodies, among others) have already expired.
At present, six of the 10 most costly drugs in the United Kingdom are biological medicines, which are synthesized from biological materials such as viruses. Their expensiveness can be attributed to the difficulty of harnessing them.
Stevens said that there are still some good news to share with the public, such as the introduction of new oral treatments to treat Hepatitis C that could save the country 50 million pounds a year. (Related: High priced anti-viral drugs do NOTHING to prevent hepatitis C, study finds.)
Stevens also commended the agency on its public service works that had proved successful over the years, as the health service nears its 70th anniversary. These include auditory brain stem implants which help give a semblance of the sensation of hearing to some children who were born with profound deafness.
The operations will be conducted by Central Manchester University hospitals and shall involve inserting a device directly against the brainstem, bypassing the auditory nerve and the cochlea, which is a portion of the inner ear that looks like a small shell. They are estimated to help around nine children yearly and are to be given a 700,000-pound investment.
The NHS also plans to introduce operations which restore eyesight to blind patients by utilizing a part of the patient’s own tooth root to steady an optical cylinder.
“The NHS has a proud history of innovation. As our 70th anniversary approaches, it is important that we do not just celebrate these often unsung achievements, but also unleash the full potential of innovation in treatment and commissioning to ensure we deliver high quality healthcare for future generations,” Stevens said.
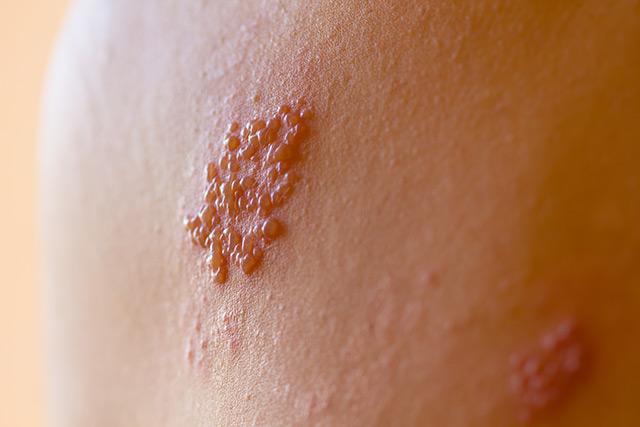
Hepatitis C is a dangerous illness that can result in life-threatening complications, such as cirrhosis or liver cancer, if left untreated. The National Institute for Health and Care Excellence recommends giving patients antiviral medicines for the ailment – those that can give specific results in as little as eight weeks.
People get infected with the virus by coming into contact with the blood of a person who is already suffering from the virus, by say, using their razor, needle, or toothbrush.
Read up on more stories such as this one at Healing.news.
Sources include:
Tagged Under: antiviral drugs, auditory brain stem implants, Big Pharma, health care, hep C treatment, hepatitis C, National Health Service